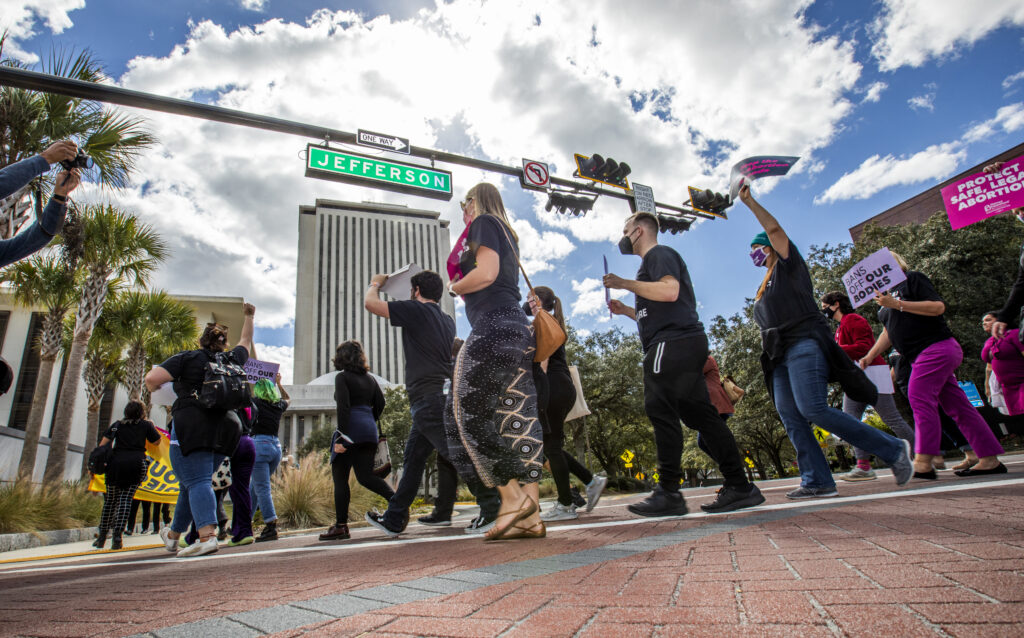Advocates for bodily autonomy march to the Florida Capitol to protest a bill before the Florida Legislature to limit abortions on Feb. 16, 2022, in Tallahassee. (Photo by Mark Wallheiser/Getty Images)
When it came to health policy, the law banning most abortions after six-weeks’ gestation was the biggest change in Florida this year. But the state agencies overseeing health safety net programs also made headlines over missteps in purging Medicaid rolls and attempts to link undocumented immigrants to strains on the health care system.
Here are our top health stories of the year.
1) Six-week abortion ban goes into effect
A landmark ruling by the Florida Supreme Court on April 1 allowed the six-week abortion ban to go into effect on May 1, cutting off access to the procedure in most cases before many people know they’re pregnant.

The state already had a 15-week ban passed in 2022, a 24-hour waiting period between appointments, and other restrictions on abortion providers. But until May 1, thousands from nearby states such as Alabama, Georgia, and Louisiana could obtain abortions in Florida.
People are still getting abortions in the state. As of Dec. 2, more than 56,000 abortions had taken place, according to the Florida Agency for Health Care Administration (AHCA). That number is down from 84,052 last year.
Doctors performing abortions and other health care providers have described the legal exceptions to the six-week ban as difficult to navigate with their patients, raising concerns about delaying life-saving care and needing to consult lawyers and law enforcement before moving forward with abortions.

In response to those concerns, Gov. Ron DeSantis and his administration have threatened disciplinary action against physicians who delay care for people who could die if they don’t get an abortion. However, doctors can also lose their medical licenses and face up to five years in prison if they perform an abortion beyond six weeks’ gestation that’s not covered under the law’s exceptions.
Nonprofit funds that help people pay for abortions face increased demand and higher costs under the six-week ban amid diminishing donations, their directors have told Florida Phoenix. The abortion-rights amendment’s loss at the polls cemented the six-week ban in the state for the foreseeable future.
2) Wrap-up of Medicaid wind-down and class action
Florida’s review of eligibility for the 5.5 million Medicaid enrollees the state amassed during the Covid-19 federal public health emergency started in 2023. Yet management of the year-long purge continued to make headlines in 2024.
During the process, supposed to wrap up by April, the state removed 1.9 million Floridians from the safety net health care program, according to a data tracker from KFF, a nonprofit health policy research group.
A week-long trial in late July in a class action accusing the state of making its notices so confusing that people couldn’t understand the reason they lost Medicaid coverage provided insight into the state’s missteps in the unwinding process. The Phoenix was one of two news outlets that covered the entire trial, detailing how AHCA and the Florida Department of Children and Families wrongfully pushed pregnant and post-partum women and their babies out of Medicaid.
While the suit’s outcome is pending, testimony from state employees and people who lost Medicaid showed DCF deficiencies in providing accurate information in its notices and through its call center, which couldn’t handle the call volume it received.
YOU MAKE OUR WORK POSSIBLE.
3) State and feds fight over KidCare rules and expansion the entire year
Children in need of the subsidized health insurance program got caught in the middle as Florida refused to comply with a Biden administration rule requiring states to provide a full 12 months of continuous coverage.
Florida filed suit against the federal Centers for Medicare and Medicaid Services in February. That suit came a month after the federal agency announced that states couldn’t remove children from CHIP (the Children’s Health Insurance Program or KidCare in Florida) for a year even if their parents missed premium payments. The subsidized version of KidCare offers coverage for $15 or $20 per month for children whose families can’t afford private insurance but earn too much to qualify for Medicaid.
Between January 2023 and July 2024, more than 21,000 kids enrolled in KidCare lost coverage because their parents missed payments, wrote Ashley Carr, Florida Healthy Kids’ chief marketing officer, to the Phoenix in August. Although both parties asked a federal appeals court to drop the suit on Dec. 13, the dispute over continuous coverage remains.
AHCA refused on Dec. 4 the Biden administration’s approval of a waiver to expand KidCare to cover children whose household income is up to 300% of the federal poverty level.
Lawmakers unanimously approved the KidCare expansion in 2023, but AHCA failed to send the federal government a waiver to enact the change. The corporation contracted to run KidCare estimated in 2023 that more than 16,000 children would qualify for the program once expanded, according to a legislative analysis.
4) Legislature approves largest health care investment in decades

Gov. DeSantis signed on March 21 a package of bills aimed at increasing the number of health care workers and promoting innovation in the industry.
The four pieces of legislation (SB 7016, SB 7018, SB 330, and SB 1758) made up the “Live Healthy” initiative, which Sen. Kathleen Passidomo spearheaded during her last session as Senate president. Live Healthy focuses on retaining and attracting health care workers to the state, creating a loan program for innovative health care projects, establishing behavioral health teaching hospitals, and providing at-home and community-based services to Floridians with disabilities.
Most recently, AHCA started the process of submitting a sweeping Medicaid waiver request that would allow the state to spend $3 billion to bolster its medical workforce over five years. Lawmakers approved Live Healthy intending to alleviate the projected physician shortage in Florida as more people move into the state and the population grows older.
5) Medicaid contracts procured
Florida Medicaid officials this year finalized new six-year contracts with the Medicaid managed care plans responsible for providing care to the millions of poor, elderly, and disabled people who rely on the program.
The six-year contracts are worth a whopping $143 billion. The multi-year agreements were more than a year in the making, with the state initially releasing its “invitation to negotiate” in April 2023. The state’s intent to award contracts briefly drew legal challenges from managed care plans that wanted to expand their existing footprints in the state’s Medicaid market or wanted to begin offering Medicaid benefits in Florida.
Ultimately, AHCA, which houses the state’s Medicaid program, awarded contracts to the managed care plans that were previously under contract with the exception of just one plan: AmeriHealth Caritas.
Community Care Plan, a managed care plan operated jointly by the North and South Broward Hospital Districts, has been under contract with the state to operate in Fort Lauderdale, its sole Medicaid region. But the new contracts extend its footprint to five Medicaid regions operating as far north as Brevard County and as far west as Lee, Collier, and Sarasota counties. Shane Strum, DeSantis’ former chief of staff, runs the North Broward Hospital District.
6) Whiplash in federal courts over gender-affirming care
Transgender Floridians and health care providers had to keep a close eye on the decisions coming out of federal courts this year regarding Florida’s ban on gender-affirming care.
Two Tallahassee federal judges delivered victories this summer for trans folks in the state, blocking Florida’s ban on puberty blockers and hormone replacement therapies for minors and restrictions for adults, as well as the coverage ban through the health insurance program for state employees.
However, those victories were short-lived. On Aug. 26, The U.S. Court of Appeals for the Eleventh Circuit sided with Florida, allowing the state’s ban on gender-affirming care for minors and limits on what kind of providers can administer hormones to adults. The same appeals court in November heard oral arguments in the suit over the state law stopping Medicaid coverage for gender dysphoria treatments.

The state employees’ lawsuit is also in limbo after Chief U.S. District Judge Mark Walker originally sided with them in August. Walker decided to halt the case on Oct. 23, awaiting a rehearing of a similar suit out of Texas on which he based his ruling.
The pending decision from the U.S. Supreme Court on Tennessee’s ban on gender-affirming care for minors could also bring consequences for the Florida suits. The conservative-leaning justices dominating the court appeared poised during the Dec. 4 hearing to allow Tennessee to enforce its law. A decision isn’t expected until June 2025.
7) Immigration intersects with health care
AHCA this year produced two reports on the immigration status of patients presenting at Florida hospitals. The first report was produced and shared with members of the Florida Legislature as mandated by law.
“High levels of uncompensated care are more associated with rural county status than illegal immigration percentages,” the first report states. “There also did not appear to be a correlation between total profitability and illegal immigration percentages. All the counties that had negative profit margins had below average illegal immigration ratios.”
AHCA’s legislative report notes the state was “not able to find any obvious correlation between the level of uncompensated care and the level of illegal aliens presenting at the hospital.”
However, the agency released a second report and dashboard that contains none of that narrative.
The dashboard includes hospital-reported data without explanation or context. For instance, it shows that the state provided $566 million in care to undocumented immigrants. The first report, however, explained that the figure was an estimate and further qualified that “it is unclear how much of that care provided to illegal aliens was uncompensated.”
Still, in a press release discusing the dashboard, AHCA Secretary Jason Weida stressed the $566 million expenditure.
“This dashboard highlights the cost of illegal immigration which puts a strain on our health care system and taxpayers here in Florida. Our hospitals and health care systems are designed to provide quality services to the citizens of the United States.”
Separately, a Tallahassee appellate court in November told AHCA it could not claw back Medicaid payments from hospitals that provided state pre-authorized emergency health care to undocumented immigrants.
8) Medical marijuana licenses awarded, challenged

Nearly 18 months after accepting 74 applications to cultivate, process, and sell medical marijuana in Florida, DeSantis’ administration announced its intent to award 22 new medical marijuana licenses.
One attorney involved in the process anticipated that 75% of the rejected applicants would file notice to challenge, either informally or formally in the state Division of Administrative Hearings. The Department of Health has not replied to the Phoenix’s request for information about challenges.
The announcement of the new licenses came weeks after the defeat of a high-profile proposed constitutional change, Amendment 3, that would have made recreational marijuana legal for adults in the state. The amendment drew the support of 57% of voters, shy of the 60% mark it needed to pass. Florida Office of Medical Marijuana Use data show that, as of Dec. 6, 890,402 patients had qualified to use medical marijuana in the state and 2,444 physicians qualified to order medical marijuana for those patients.
Florida law lists 13 conditions that qualify patients for medical marijuana treatment: cancer, epilepsy, glaucoma, positive status for human immunodeficiency virus (HIV) or acquired immune deficiency syndrome (AIDS), post‐traumatic stress disorder (PTSD), amyotrophic lateral sclerosis, Crohn’s disease, Parkinson’s disease, and multiple sclerosis.
Statutes also allow patients with “medical conditions of the same kind or class” as the above conditions to qualify. Moreover, patients who are terminal and who have chronic nonmalignant pain also can qualify for medical marijuana.
The Board of Medicine and Board of Osteopathic Medicine released a report earlier this year that shows 40% of the patients qualify for treatment because of a PTSD diagnosis. Another 29.3% qualify under the “medical conditions of the same kind of class” diagnosis. The notice of intent to award licenses is expected to be challenged.
GET THE MORNING HEADLINES.